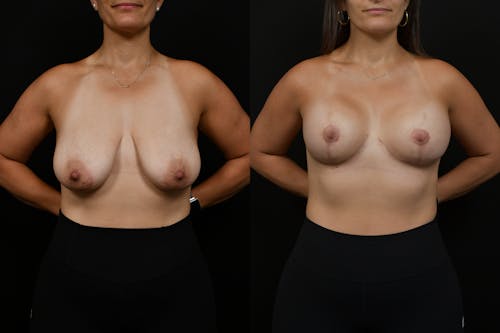
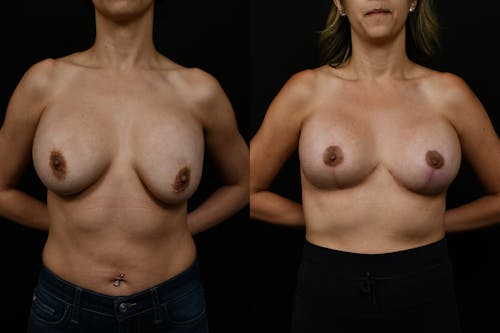
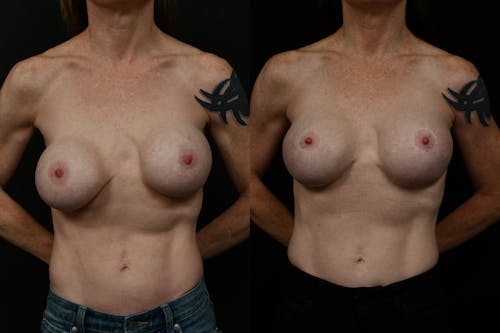
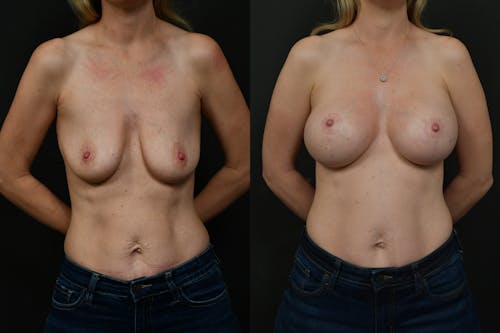
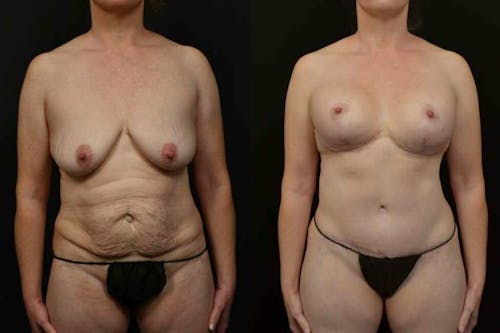
The reductive augmentation procedure is Changes’ signature solution for large-breasted women who want to have a long-lasting result with an improved breast shape. This technique makes their breasts perkier with upper pole fullness that will last a lifetime since the lower part of the breast tissue is removed.
Operative Technique
The Changes Plastic Surgery team developed this novel technique to find a better solution for breast reduction patients who grapple with daily challenges due to breast size and shape. This approach to breast reduction aims not only to alleviate physical discomfort but also to enhance overall appearance.
By meticulously removing excess inferior and lateral tissue and strategically placing a small-volume breast implant beneath the chest muscle, our surgeons achieve unparalleled aesthetic outcomes. Though unconventional, this method addresses sagging and ensures longer-lasting results.
Despite initial hesitation, the addition of a breast implant counteracts tissue drooping over time, resulting in enhanced cleavage and a youthful, symmetrical appearance. This innovative technique exemplifies personalized care and artistic precision, transforming aged, sagging breasts into perky, youthful contours.